Retinal Tear & Detachments
Diseases of the Retina/Vitreous: Retinal Tears and Detachments
What are Retinal Tears and Detachments?
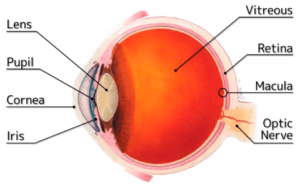
The retina is the light-sensitive layer of tissue that lines the back wall of the eye. The retina is responsible for vision. When the retina detaches, it is lifted or pulled from its normal position. If not promptly treated, retinal detachment can cause permanent vision loss.
In some cases, there may be small areas of the retina that are torn open. These areas, called retinal tears or retinal breaks, can lead to retinal detachment.
What causes Retinal Tears and Detachments?
What causes Retinal Tears and Detachments?
Retinal detachments can develop at any age, but they are more common in people over the age of 60. A retinal detachment can develop for no identifiable reason. However, several factors increase the risk of developing a retinal detachment. Myopia (being very nearsighted), eye inflammation or injury, a family history of retinal detachments or tears, prior eye surgery, and other eye diseases can increase the risk of retinal detachment.
Typically, a retinal detachment develops after a retinal tear or hole occurs.
What are the Symptoms of Retinal Tears and Detachments
What are the Symptoms of Retinal Tears and Detachments?
 Warning symptoms of a retinal detachment or retinal tear include a sudden or gradual increase in the number of floaters (blobs, black spots, or spider webs moving through the vision), flashes of light in the eye, or the appearance of a veil or curtain over the field of vision.
Warning symptoms of a retinal detachment or retinal tear include a sudden or gradual increase in the number of floaters (blobs, black spots, or spider webs moving through the vision), flashes of light in the eye, or the appearance of a veil or curtain over the field of vision.
Video: Flashes and Floaters
What are the Treatment Options?
What are the Treatment Options?
The common treatment options for retinal holes and tears are laser treatment, which “fuses” the retina back into place, or a cryopexy, which “freezes” the area around the hole. These procedures usually are done in the retina doctor’s office and are accompanied by little discomfort. You may be advised to limit your physical activity for a short time. Your eye may be blurry and red for several days after treatment.
Retinal detachments are treated with surgery performed on an outpatient basis.
One procedure, called pneumatoretinopexy is done in the doctor’s office. This procedure uses a gas bubble to push the retina back into place. In some cases, a “scleral buckle” or tiny silicone band, is attached to the outside of the eyeball to gently push the wall of the eye against the detached retina and hold the retina in position. This procedure is done in the operating room on an outpatient basis.
Your retina doctor may recommend an operation called a “vitrectomy” in which the clear jelly-like substance that fills the eyeball (vitreous) is removed and replaced with a gas bubble or saline-like fluid. Following surgery, patients may need to limit activity and maintain a certain head position to help the retina reattach.
Early treatment usually can improve the vision of most patients with retinal detachment. Some patients, however, will need more than one procedure to repair the damage.
Video: Vitrectomy
Video: Scleral Buckle
Video: Pneumatic Retinopexy
What You Can Do to Protect Your Vision
What You Can Do to Protect Your Vision
Early detection and treatment, when indicated, is the best way to prevent vision loss. Regular yearly examinations by your eye doctor are extremely important because eye problems can develop at any age. Urgent evaluation is warranted if you have a significant increase in light flashes, floaters, or a cloud in vision.
Making the Most of Your Remaining Vision
Making the Most of Your Remaining Vision
Early detection and treatment may reduce the loss of vision from Diabetic Retinopathy. However, if some loss of vision should occur, it doesn’t have to rob you of life’s simplest pleasures if you learn how to use your remaining eyesight to see your best. Low vision aids, special lenses, or electronic systems and training can maximize your ability to read and perform other activities.
The Low Vision Rehabilitation Center of Retina Consultants of Southwest Florida can give you more information about the training and devices available.

 Warning symptoms of a retinal detachment or retinal tear include a sudden or gradual increase in the number of floaters (blobs, black spots, or spider webs moving through the vision), flashes of light in the eye, or the appearance of a veil or curtain over the field of vision.
Warning symptoms of a retinal detachment or retinal tear include a sudden or gradual increase in the number of floaters (blobs, black spots, or spider webs moving through the vision), flashes of light in the eye, or the appearance of a veil or curtain over the field of vision.